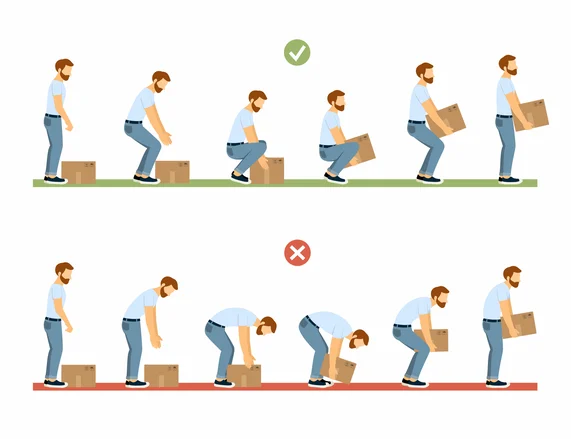
If you’ve ever spent time around caregivers, nurses, or anyone who works closely with patients, you’ve probably seen it without realizing it has a name. Rounded shoulders. A bent neck. A slight forward fold that shows up during transfers, dressing, or even simple conversations at bedside. This posture is often called the caregiver stoop, and while it looks harmless, it’s one of the biggest contributors to long-term pain and injury in care environments.
The caregiver stoop usually doesn’t come from laziness or poor training. It develops slowly, almost invisibly. Caregivers lean forward to be closer, to be gentle, to be reassuring. They bend instead of lowering their center of gravity because it feels faster and more natural in the moment. Over time, those small choices stack up. The spine takes the load, shoulders tighten, and the body starts working against itself.
This is where the approach taught by Eastern Ergonomics really stands out. Instead of telling people to “stand up straight” or memorize rigid lifting rules, their method focuses on how the body is designed to move under load. The goal isn’t perfect posture. It’s efficient, protective movement that works in real caregiving situations.
The fix for the caregiver stoop starts with awareness. Most caregivers don’t realize how often they hinge at the upper back instead of the hips. When the bend comes from the spine, the muscles fatigue quickly and the joints take stress they’re not meant to handle repeatedly. Over time, this leads to chronic back pain, neck tension, and shoulder injuries that feel unavoidable in the profession.
Protective ergonomic training reframes the movement. Instead of folding forward, caregivers learn to bring their whole body closer to the task. That might mean stepping in, widening the stance slightly, and lowering through the legs rather than collapsing the upper body. The spine stays more neutral, the hips and legs share the load, and the caregiver feels more stable instead of strained.
What’s powerful about this shift is how immediate the difference feels. Caregivers often report less tension after just a few adjustments. Movements feel grounded rather than rushed. There’s less fear of “throwing out” their back, which alone changes how confidently they approach physical tasks.
Another key part of fixing the caregiver stoop is timing. Many injuries happen not during heavy lifts, but during small, repetitive movements done while distracted or fatigued. Training emphasizes slowing down just enough to reset posture before engaging. That pause might last only a second, but it’s enough to protect the body from unnecessary stress.
This approach has been refined and taught by professionals like Ben Couch, who combine ergonomic science with real-world movement principles. The focus isn’t theory for theory’s sake. It’s practical, repeatable habits that caregivers can use in tight spaces, unpredictable situations, and emotionally demanding moments.
The benefits go beyond physical health. When caregivers aren’t constantly bracing for pain, their energy shifts. They’re more present with patients. Interactions feel calmer and more controlled. Patients sense that confidence and respond to it, which can make transfers and assistance smoother on both sides.
Over weeks and months, fixing the caregiver stoop pays off in ways organizations can measure. Fewer injury reports. Less missed work. Lower turnover. But just as important, caregivers feel respected and supported when they’re given tools that protect their bodies, not just instructions to “be careful.”
The caregiver stoop isn’t a personal failure. It’s a natural response to demanding work done without the right movement framework. The fix isn’t about forcing posture or adding strain. It’s about learning to move smarter, closer, and with intention.
Once that shift happens, caregiving stops feeling like something the body must endure and starts feeling like something it can sustain.